National Eczema week was marked this month so we're looking at how to control this skin condition that is so common in childhood, plus we've plenty of tips to make your child more comfortable.
What is eczema?
There are different kinds of eczema but the most common is known as atopic eczema (AE), also known as atopic dermatitis. (The words eczema and dermatitis mean the same thing.)
With atopic eczema, the skin becomes inflamed and the skin is itchy, dry, cracked and red.
It usually appears behind the knees, on the elbows and on the face and scalp, though it may cause patches on other parts of the body, too.
It is most common in children, and affects boys and girls equally, often appearing before they are a year old.
It is thought up to 20% of infants in the UK will have eczema at some stage but it often disappears later in childhood but can return in teenage or early adult years.
Why does my child have it?
A number of factors can contribute towards the development of AE including how susceptible a patient may be and external, environmental factors.
Skin that is prone to eczema often has structural changes or problems within the skin barrier making it difficult for the skin to keep in moisture and stay hydrated while at the same time making it more vulnerable to irritants and infection.
This structural problem of the skin barrier is caused by a gene alteration which can run in families.
If one or both parents have eczema it is much more likely their children will develop eczema as well.
Environmental factors can include contact with soaps, detergents, chemicals, bacteria, viruses or exposure to allergens.
Eczema cannot be caught from other people.
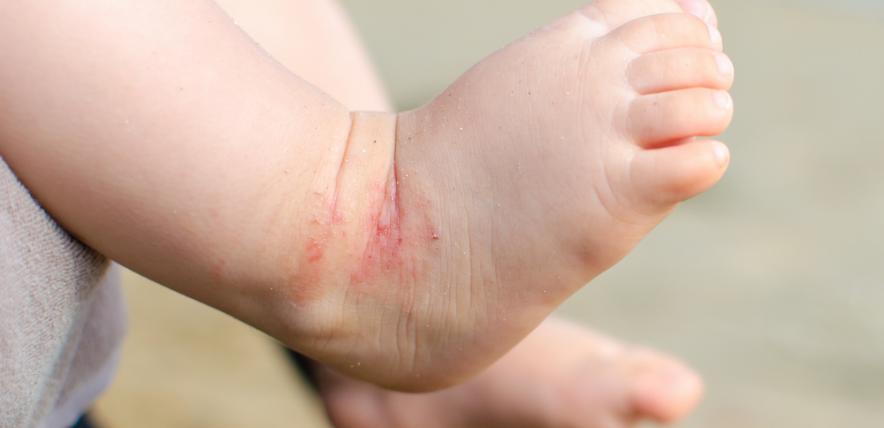
What does atopic eczema look like?
Patches of eczema commonly occur in the creases of the elbow and behind the knees, at the wrist and at the neck. However other coin-shaped areas of inflammation can appear on arms and legs as well.
The affected area of skin will usually be red and dry and may well have scratch marks with perhaps bleeding.
If your child has repeatedly been scratching a particular area, the skin may thicken and may itch even more.
In severe cases affected area may weep and have small water blisters.
What are the symptoms?
The most common symptom is itching. If the itching is really bad it may keep your child up at night making them tired and grumpy.
Eczema often comes and goes. Sometimes you will see your child have a ‘flare up’ when their skin gets worse and then the eczema will clear up for a while.
Flare ups
Often it is unclear and unknown why a flare up occurs but some of the reasons may be due to:
- Being ill, for example with a cold
- Bacterial infection or viruses
- Heat, dust, woolly clothes, animal fur or irritants such as soap and detergent can cause flare ups
- Teething
- In rare cases, a food allergy may cause a flare up.
How do I treat it?
The main treatment for atopic eczema is ‘emollient therapy’ which means regularly applying a moisturiser, known as an emollient, at least twice a day.
Use the greasiest one you can find and that you don’t mind using.
Aqueous creams can irritate the skin and make it worse so don’t use them — use moisturiser.
You should also stop using soaps, shower gels and bubble bath.
Some dermatologists suggest fewer baths a week if possible. This may not be possible if you have a baby that needs washing every day because of dirty nappies etc but shorter baths or showering them off with a hand shower can help the skin rather than sitting and soaking in water for long periods of time which further dries skin out. Hot baths or showers dry out the skin even more — but very hot water should not be used for bathing babies and very young children anyway.
In more serious cases of eczema, GPs can prescribe a gentle steroid cream to bring it under control for a while but these shouldn’t be overused as they can thin the skin. Your doctor can advise you on this.
To stop your child scratching their skin at night, put mittens, gloves or even socks over their hands when they sleep.
Can atopic eczema be cured?
Unfortunately it cannot be cured but it can be managed and controlled with care and creams.
How do I get my child properly diagnosed?
Your health visitor should be able to recognise eczema or if you don’t have a health visitor, take them to a GP. In most cases, health workers will be able to identify the condition visually without the need for swabs or tests. If there is a risk of infection then the skin will be swabbed.
Tips from the British Association of Dermatologists
Treat eczema early — the more severe it becomes, the more difficult it is to control.
Moisturise the skin as often as possible, at least twice a day. The most greasy, non-perfumed moisturiser tolerated is best. This is the most important part of your skin care. Smooth it on in the direction of hair growth. To avoid infection, don’t use your fingers to keep taking moisturiser out of the pot. It is best to take the required amount out with a spoon or spatula and put this on a saucer. Then use clean, washed hands to apply the emollient.
Avoid soap, bubble baths and shower gels. Wash with a moisturiser instead of soap (known as a soap substitute). For example an emollient such as Epaderm can be mixed with water to make a soft, greasy liquid and used like soap to wash the skin.
Dress your child in materials such as cotton and avoid wool next to the skin as it can make it feel itchy.
Avoid close contact with anyone who has an active cold sore as patients with eczema are at risk of getting a widespread cold sore infection.
Do not keep pets if your child shows signs of being allergic to them.
Keep cool. Overheating can make eczema itch more.
Wash clothes with a non-biological washing powder and use a double rinse cycle to remove detergent residues from the clothing.
For more information download the Association's full leaflet
This article is for information purposes only and should not be used as a substitute for professional medical help. If you or your child is unwell you should consult a medical professional.